What is the Function of Intervertebral Discs?
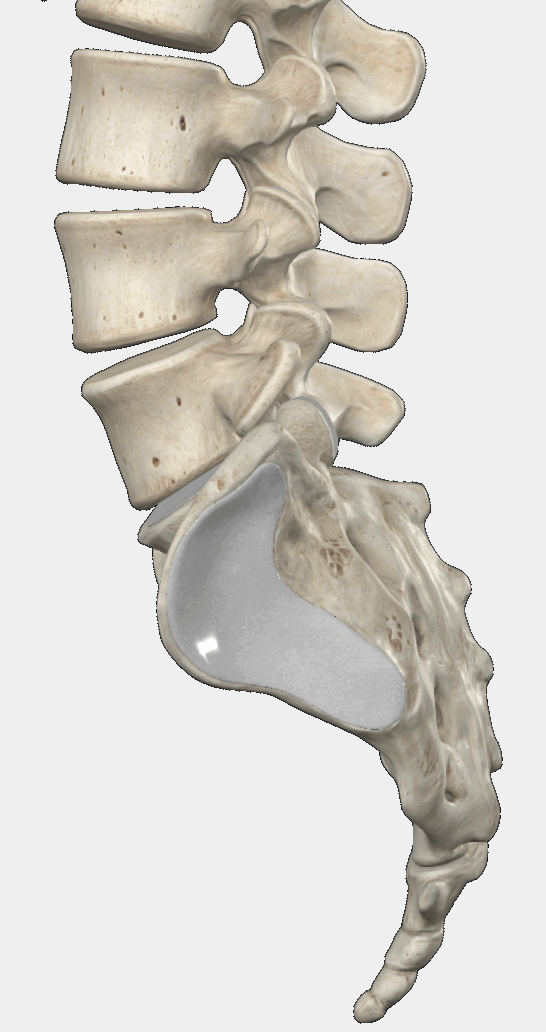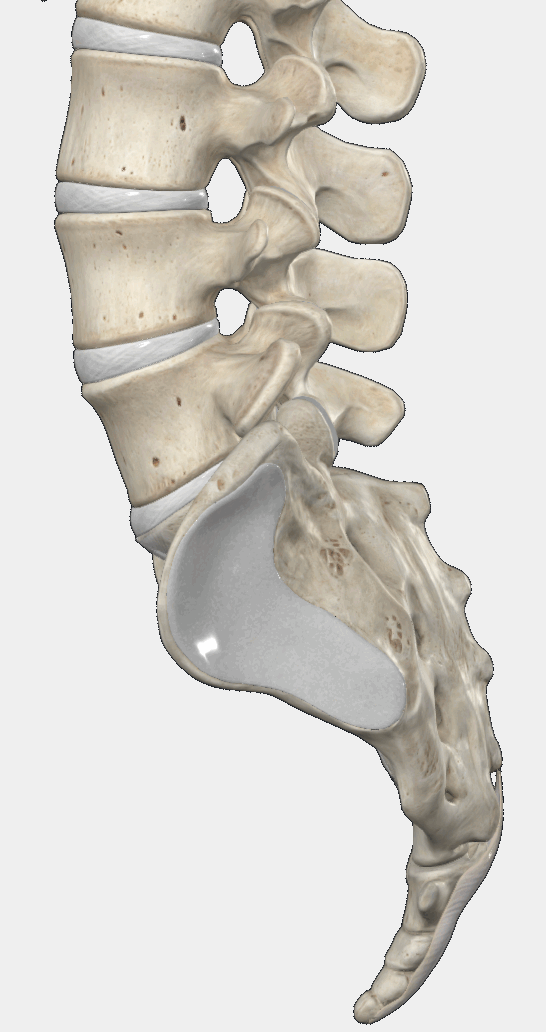
Intervertebral discs act as cushions between the vertebrae of the spine. They consist of a tough outer fibrous layer and a soft, gel-like inner core.
A simple way to imagine them is like small jelly-filled donuts—perfectly sized to fit between the vertebrae and absorb mechanical stress.
How Does a Disc Bulge Develop?
Over time, intervertebral discs undergo age-related changes: they lose hydration, become stiffer, and less flexible.
As a result, the outer layer of the disc may begin to bulge evenly around its circumference—similar to a burger patty that is slightly too large for its bun. This is called a disc bulge.
A bulging disc does not necessarily involve the entire circumference, but typically at least a quarter or even half of it. In these cases, only the outer fibrous layer is affected.
This is not considered a disc herniation, and it may not cause any symptoms.
What Causes a Disc Herniation?
A disc herniation occurs when the tough outer layer of the disc develops a tear, allowing the softer inner gel to protrude outward.
This can be compared to a burger patty pushing out through a small gap in the bun—localized, but more pronounced.
This condition is a result of spinal instability, as discussed in the general section. Due to micro-instability, the disc becomes overloaded and bulges at its weakest point.
Symptoms depend on what the protruding disc is affecting:
-
It may be completely asymptomatic
-
It may cause discogenic (disc-related) pain
-
It may compress a nerve root, leading to radicular pain
It is important to note that a disc herniation seen on MRI is not always the source of pain. Many people have disc herniations—or even extrusions—visible on imaging without experiencing any back or neck pain¹.
This is why a thorough clinical evaluation is essential. Without an accurate diagnosis, effective treatment is not possible.
How Can it be Treated?
Treatment of a disc herniation depends on symptom severity and the extent of nerve involvement.
At PSI Pain Clinic, our goal is to reduce pain using targeted, minimally invasive procedures—while avoiding major spine surgery whenever possible. A range of modern treatment options is available:
A targeted injection into the epidural space, delivering steroids and other medications directly near the affected nerve root.
This helps reduce inflammation and relieve pain.
A more precise injection technique in which medication is delivered directly to the specific nerve root affected by the disc herniation.
A minimally invasive procedure used to break down scar tissue in the epidural space and treat nerve roots compressed by a disc herniation.
The goal is to release irritated nerves and improve the condition of the affected area.
Endoscopic spine surgery is a modern, minimally invasive procedure in which the nerve-compressing lesion is removed through a small 1–1.5 cm incision using camera guidance. The goal of the intervention is to relieve nerve pressure, reduce pain, and ensure a rapid recovery.
The procedure is performed under sedation and does not require general anesthesia, resulting in minimal tissue trauma. The surgery typically takes 60–120 minutes and is carried out as a day-case procedure, meaning patients can often go home on the same day.
It can be a gentle and effective solution for patients whose symptoms have not improved with conservative treatment.
Source:
1. M C Jensen, M N Brant-Zawadzki, N Obuchowski, M T Modic, D Malkasian JSR. Magnetic Resonance Imaging of the Lumbar Spine in People Without Back Pain. N Engl J Med. 1994 Jul;331(2):69–73.


