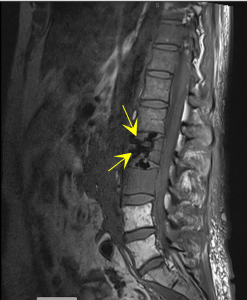
What is a Vertebral Compression Fracture?
A vertebral compression fracture most commonly occurs in the front part of the vertebra (vertebral body), where the bone collapses due to weakened structural integrity—even as a result of minimal force.
The most common underlying causes of weakened bone structure include:
-
Osteoporosis
-
Cancer-related bone involvement (metastasis)
-
Less commonly: inflammation or genetic bone disorders
How Does a Vertebral Compression Fracture Develop?
In vertebrae with compromised bone structure, even minor trauma can lead to collapse.
For example, in cases of cancer-related bone changes, the vertebra may become structurally weak and prone to fracture under normal or minimal load.
What are the Symptoms?
Vertebral compression fractures typically cause severe, localized pain. However, pain may also radiate to other areas away from the fracture site.
Pain usually:
-
Worsens with movement or weight-bearing
-
Improves when lying down and resting
In more severe cases, vertebral collapse may lead to:
-
Nerve root compression → numbness, radiating pain, weakness
-
Spinal canal narrowing → potential spinal cord compression
If nerve roots are affected, symptoms may include sensory disturbances, limb weakness, or loss of coordination.
If the spinal cord is compressed, more serious symptoms can develop, such as:
-
Difficulty walking
-
Loss of strength or paralysis
-
Bladder or bowel dysfunction
-
Reduced respiratory function (in severe cases)
Over time, vertebral deformity may lead to spinal curvature (kyphosis, or “hunched posture”), which can cause additional musculoskeletal problems.
How Is it Diagnosed?
After clinical evaluation, vertebral compression fractures are diagnosed using imaging studies such as:
-
X-ray
-
CT scan
-
MRI
-
Bone scintigraphy
These tests also help determine whether the fracture is recent or old, which is crucial for selecting the appropriate treatment.
How Is it Treated?
Conservative Treatment
If the fracture:
-
Does not affect mobility
-
Does not cause neurological symptoms
-
Is unlikely to worsen spinal biomechanics
-
And pain is manageable with medication
Then conservative treatment is recommended, including:
-
Hydrotherapy
-
External bracing
In elderly patients, prolonged bed rest is not recommended due to the risk of complications such as pneumonia, thrombosis, or pulmonary embolism.
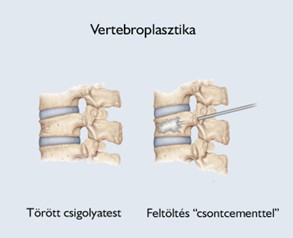
Vertebroplasty
Vertebroplasty is a minimally invasive procedure in which medical cement is injected into the vertebral body through a needle to stabilize the fracture.
Open Spine Surgery
In a small number of cases, open surgery may be required—particularly if bone fragments compress the spinal cord or nerve roots.
When is Vertebroplasty Indicated?
Early treatment is important to prevent progression of spinal deformity.
If conservative treatment fails, or if pain worsens, a stabilizing procedure may be necessary to reduce pain and prevent further collapse. One such option is vertebroplasty.
The most appropriate surgical technique is determined by the specialist based on the patient’s medical history and imaging findings.
What Happens if it is Left Untreated?
If a vertebral compression fracture is not treated—either conservatively or surgically:
-
Pain may persist or worsen
-
Spinal deformity may progress
The collapsed vertebra may also compress nerve roots or the spinal cord, leading to:
-
Numbness, weakness, or paralysis
-
Walking difficulties
-
Bladder and bowel dysfunction
-
Respiratory problems (in severe cases)